LUNG ABSCESS AND AIR-FLUID LEVEL
Abstract
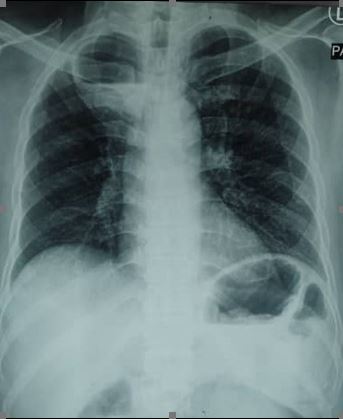
A 49-year-old male, chronic smoker with a background of diabetes mellitus and hypertension presented with a one-month history of productive cough, reduced appetite, and weight loss. He reported no history of alcoholism, fever, breathlessness, haemoptysis, and chest pain. The chest radiograph showed a cavitating lung lesion with air-fluid level in the right upper lobe (figure-1). CT of the thorax later revealed a well-defined irregular thin-wall enhancing cavitating lesion with air-fluid level within (7.0×6.5×5.6 cm), seen at the apical segment of the right upper lobe, which was indicative of lung abscess (figure-2). There were no enlarged hilar or mediastinal lymph nodes. The workup for pulmonary tuberculosis and malignancy was negative. He was administered with intravenous amoxicillin-clavulanic acid 1.2 g every 8 hours. A repeat thoracic CT done at a 2-week interval did not show any radiological improvement. In view of poor response to antimicrobial therapy, CT-guided percutaneous catheter drainage was attempted but there was no output from the drain. The sputum culture yielded Klebsiella pneumoniae and Serratia marcescens, susceptible to piperacillin-tazobactam and cefuroxime. He received intravenous piperacillin-tazobactam for 2 weeks, followed by a prolonged course of oral cefuroxime for 3 months. The lung abscess completely resolved upon completion of antibiotic therapy.
References
Kuhajda I, Zarogoulidis K, Tsirgogianni K, Tsavlis D, Kioumis I, Kosmidis C, et al. Lung abscess-etiology, diagnostic and treatment options. Ann Transl Med 2015;3(13):183.
Gadkowski LB, Stout JE. Cavitary pulmonary disease. Clin Microbiol Rev 2008;21(2):305-33.
Yazbeck MF, Dahdel M, Kalra A, Browne AS, Pratter MR. Lung Abscess: update on microbiology and management. Am J Ther 2014;21(3):217-21.
Downloads
Published
How to Cite
Issue
Section
License
Journal of Ayub Medical College, Abbottabad is an OPEN ACCESS JOURNAL which means that all content is FREELY available without charge to all users whether registered with the journal or not. The work published by J Ayub Med Coll Abbottabad is licensed and distributed under the creative commons License CC BY ND Attribution-NoDerivs. Material printed in this journal is OPEN to access, and are FREE for use in academic and research work with proper citation. J Ayub Med Coll Abbottabad accepts only original material for publication with the understanding that except for abstracts, no part of the data has been published or will be submitted for publication elsewhere before appearing in J Ayub Med Coll Abbottabad. The Editorial Board of J Ayub Med Coll Abbottabad makes every effort to ensure the accuracy and authenticity of material printed in J Ayub Med Coll Abbottabad. However, conclusions and statements expressed are views of the authors and do not reflect the opinion/policy of J Ayub Med Coll Abbottabad or the Editorial Board.
USERS are allowed to read, download, copy, distribute, print, search, or link to the full texts of the articles, or use them for any other lawful purpose, without asking prior permission from the publisher or the author. This is in accordance with the BOAI definition of open access.
AUTHORS retain the rights of free downloading/unlimited e-print of full text and sharing/disseminating the article without any restriction, by any means including twitter, scholarly collaboration networks such as ResearchGate, Academia.eu, and social media sites such as Twitter, LinkedIn, Google Scholar and any other professional or academic networking site.









